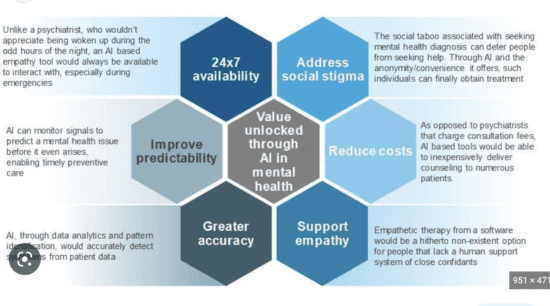
In the last post we discussed how AI can help with breakthrough approaches to managing mental health as this has been a difficult field within healthcare to show rapid progress. Brain is one of the most challenging organs to de-code for medical researchers. This is due to its physical complexity and the billions of connections that result in the management of our thinking, feelings, emotions, etc. Large data, multi-dimensional data! Sounds like a problem well-suited for AI!!
One of the goals of AI research is to categorize patients’ diagnoses into different condition subgroups so that physicians are able to provide personalized treatment. In a study published in Translational Psychiatry, researchers used machine learning to identify two forms of post-traumatic stress disorder in veterans, a mild form with relatively few symptoms and a chronic, severe form in which patients experienced high levels of depression and anxiety.
Using machine learning, it may be possible to identify as many as five different subcategories of PTSD, including mild, severe, cognitive functioning impaired, depressed and anxious and dissociative. Researchers will also focus on molecular and brain circuit markers, genes and the products of genes, such as proteins and metabolites, with the aim of understanding how they’re associated with each of the different forms of PTSD. All of this is made possible by using AI to sift through the massive amounts of data and identify patterns and associations.
AI is also being used to incorporate sensor data through wearable health technologies to better manage patients. For example, mental health providers have two choices: they can either ask patients to self-report how they’ve been sleeping or they can access their sleeping data from devices like smartwatches. This is important because there’s a big disconnect between how we think we sleep versus how we actually do sleep. If we’re able to use a combination of smartwatches and AI technology then we might be able to gain a more subjective look at how patients are sleeping. Accurately tracking sleep patterns could give providers an indication of which patients with bipolar disorder might be more at risk of experiencing an episode of mania, allowing for adjustments in medication.